Safe, Efficient, and Easy to Use
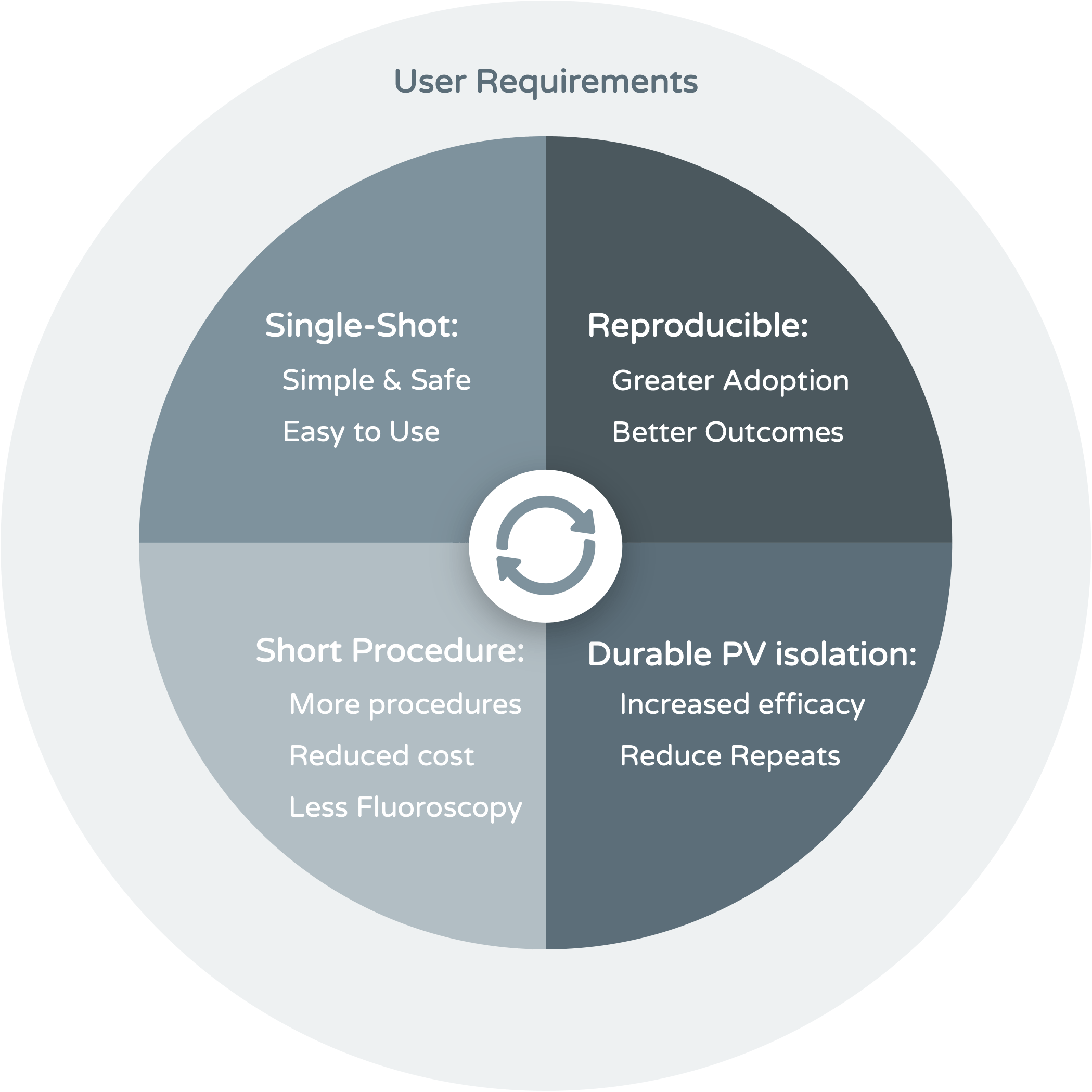
Clinicians seek tools that are safe, easy to use, effective, and efficient.
Easy to use
Effective
Efficient
Understanding the market’s needs, we focused on designing a safe, efficient, and easy to use “single-shot” ablation catheter to allow for the delivery of durable and longstanding ablation lesions. Unlike balloon-based solutions, EPF's array of electrodes does not occlude pulmonary venous blood flow or have the risk of gaps due to poor tissue contact.
Our catheter specifically addresses the greatest challenges faced - catheter stability and the delivery of continuous transmural lesions.
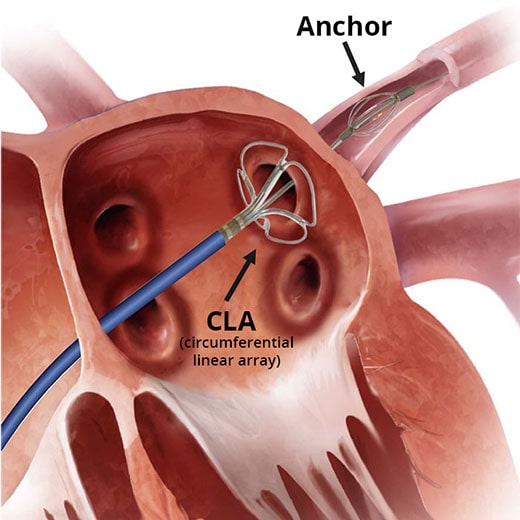
Catheter Design
The features of our unique anchor AND electrode design include:
Catheter Features
Interested in learning more about our innovative “single-shot” catheter ablation system?

